What is Tendinopathy?
Many athletes, people over 40, and workers who perform repetitive tasks experience some degree of Tendinopathy during their lives. Starting out, a healthy tendon is a flexible, rope-like tissue that attaches muscles to bones and allows for movement. Then, at some point, either from a sudden injury or repeating a task countless times, a tendon becomes damaged and causes a person pain, swelling, or movement dysfunctions (tendinopathy).
One of the main problems we see as Physical Therapists when it comes to Tendinopathy is that most people need to recognize how minor or severe the damage to their tendon actually is. Without a proper diagnosis and treatment plan, mild discomfort and stiffness can quickly turn into more chronic pain and disability. For this reason, we decided to provide a comprehensive and easy-to-follow look at Tendinopathy. This article will include:
- The four stages of tendinopathy
- Tendinopathy pathology and related symptoms
- The five most common types of tendinopathies we see at Balanced Physical Therapy
- How Physical Therapists can treat tendinopathy
- As well as general guidelines for exercise when dealing with a tendon injury
Stages of Tendinopathy
As previously mentioned in the intro, a healthy tendon is firm, not painful, has no swelling, and has an average temperature (not warm/hot to the touch). As damage to a tendon begins and continues to compound, a person will experience one or more of the Four Stages of Tendinopathy.
Stage 1: Reactive Tendinopathy
- This initial stage occurs when the tendon is exposed to excessive or repetitive stress or sudden increases in physical activity.
- Microscopic changes in the tendon structure occur, including collagen disorganization and increased cell activity.
- Symptoms may include mild pain, stiffness, and discomfort in the affected area.
- In this stage, the tendon may still have the potential to heal and recover with appropriate rest and conservative treatment.
Stage 2: Tendon Disrepair
- If the stress or strain on the tendon continues without adequate rest or treatment, the condition may progress to the disrepair phase.
- In this phase, there is more significant damage to the tendon tissue, including further collagen disorganization, the accumulation of abnormal blood vessels, and ongoing cell proliferation.
- Pain and functional impairment may become more noticeable and persistent.
- Treatment at this stage typically involves a combination of rest, physical therapy, and possibly medications to manage pain and inflammation.
Stage 3: Degenerative Tendinopathy
- In this stage, there is a more pronounced breakdown of tendon tissue, with the development of degenerative changes, including the formation of tendon nodules or areas of tissue thickening.
- The tendon structure becomes further compromised, and the tendon may lose some of its elasticity and strength.
- Pain and functional limitations can be more severe at this stage.
- Treatment may require more intensive physical therapy focused on eccentric exercises, other specialized techniques, and potential interventions like corticosteroid injections or other regenerative therapies.
Stage 4: Tendon Rupture
- The final stage of tendinopathy is tendon rupture, where the tendon may partially or completely tear.
- This can result from the cumulative damage and weakening of the tendon over time.
- A complete tendon rupture often requires surgical intervention to repair, while partial tears may be managed conservatively or surgically depending on their severity.
- Recovery from a tendon rupture can be lengthy, and rehabilitation is crucial to restore function and strength.
Most Common Types of Tendinopathies
At Balanced Physical Therapy, the four most common types of tendinopathies that we treat include:
Shoulder/Rotator Cuff Tendinopathy
- Supraspinatus Tendinopathy is a specific tendinopathy that affects the supraspinatus tendon (part of the shoulder rotator cuff). It often leads to pain and limited shoulder mobility, especially when raising the arm.
- This type of injury risk factors include poor shoulder mechanics (especially with weight lifters), getting older (risk typically begins at age 40 and peaks around 80), previous shoulder dislocations, or chronic shoulder impingement.
Elbow Tendinopathy
- Tennis Elbow (Lateral Epicondylitis) is tendinopathy that affects the outer part of the elbow. It is often caused by repetitive arm motions, such as those in tennis or other racquet sports. Pain and weakness in the forearm are common symptoms.
- Golfer Elbow (Medial Epicondylitis) is similar to tennis elbow but affects the inner part of the elbow. It often occurs due to repetitive gripping or wrist flexion, leading to pain and weakness in the forearm.
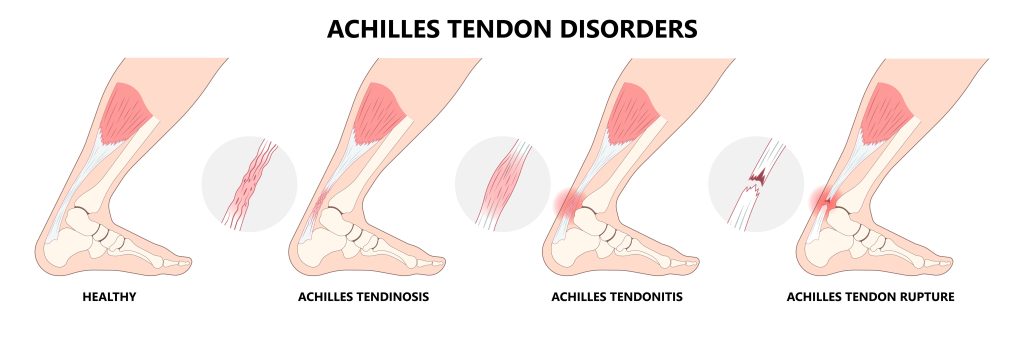
Achilles Tendinopathy
- This affects the Achilles tendon, which connects the calf muscles to the heel bone. It often results from overuse or excessive strain and can cause pain and stiffness in the back of the ankle.
- This injury is most often a result of a sudden increase in physical activity, overuse, foot pronation, obesity, or excessive training that includes hills and poor shock absorption.
Patellar Tendinopathy ( Jumper’s Knee)
- This condition affects the patellar tendon, which connects the kneecap (patella) to the shinbone (tibia). It is common in athletes who engage in jumping sports and can cause knee pain, especially just below the kneecap.
Biceps Tendinopathy
- The long head of the biceps tendon runs through the front of the shoulder and can be susceptible to tendinopathy. This condition may cause pain and discomfort in the front of the shoulder and upper arm.
Rehabbing a Tendon Injury
If you caught your tendinopathy symptoms early on, either in Stage 1 or 2 of Tendinopathy, you can fully recover as quickly as a few days or weeks. More severe tendinopathies can sometimes take anywhere between two to six months. The good news for many people with tendinopathy is that they can fully recover without surgery.
Because tendinopathy is a progressive condition, early diagnosis and appropriate treatment will be vital in reaching favorable outcomes. Suppose you are experiencing pain (especially when moving), swelling, stiffness/restricted mobility, muscle weakness, and/or burning/warm sensation. In that case, you should see your primary care physician, physical therapist, or any other specialist who works with muscle and bone injuries.
Your doctor may recommend some self-care treatments that include pausing the activity that triggered your symptoms, decreasing the intensity of the activity causing you problems, and/or icing your affected area to help reduce swelling/pain.
For others, a more professional approach, like physical therapy, may be necessary to rehab a tendon injury. Specific physical therapy treatments for tendinopathy can vary depending on the location and severity of the condition, but some common approaches include:
- Education and Activity Modification: The first step is often educating the patient about their condition and how to modify their activities to reduce stress on the affected tendon. This may involve avoiding specific movements or activities that exacerbate symptoms.
- Pain Management: Physical therapists may use modalities such as ice, heat, or ultrasound to help manage pain and reduce inflammation in the affected area.
- Stretching and Range of Motion Exercises: Gentle stretching exercises can help improve the flexibility of the tendon and the surrounding muscles. Range of motion exercises are also essential to maintain joint mobility.
- Strengthening Exercises: Gradual strengthening of the muscles around the affected tendon is crucial. Strengthening exercises help support the tendon and promote healing. This may involve eccentric exercises, where the muscle is lengthening while under load.
- Manual Therapy: Hands-on techniques, such as massage, myofascial release, and joint mobilizations, can help reduce muscle tension and improve blood flow to the affected area.
- Taping and Bracing: Taping techniques like kinesiology tape or braces may support the affected tendon and help reduce strain during movement.
- Ergonomic and Biomechanical Assessments: Evaluating and correcting any ergonomic or biomechanical issues that may contribute to tendinopathy is essential. This can involve analyzing posture and movement patterns and making adjustments as needed.
- Modalities: Depending on the specific case, other modalities like electrical stimulation, ultrasound, or laser therapy may be used to promote healing and reduce pain.
- Functional Training: As the patient progresses, functional exercises that mimic real-life activities may be incorporated to ensure that the individual can safely return to daily activities and sports.
- Home Exercise Program: Physical therapists often provide patients with a tailored home exercise program to continue their rehabilitation outside clinic visits.